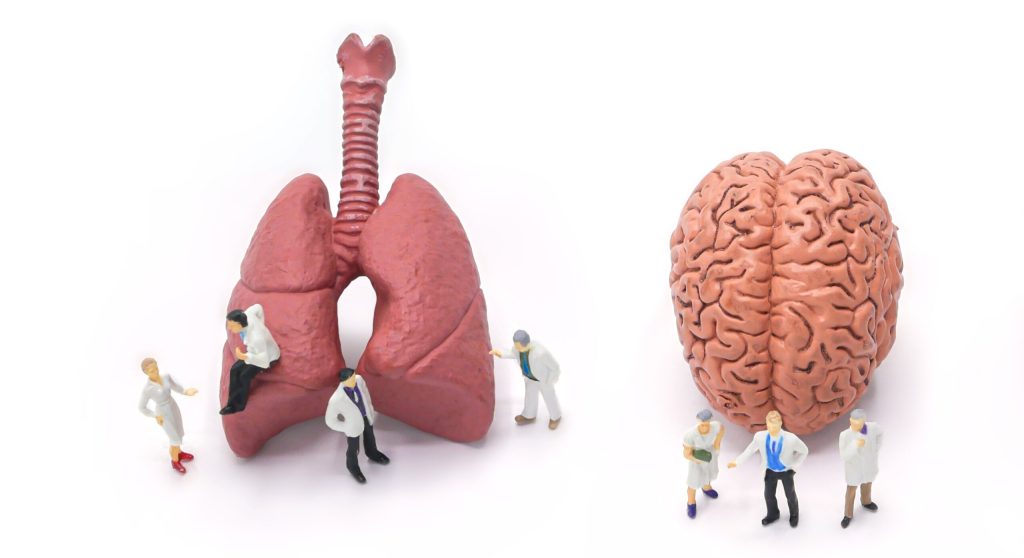
Previously unknown interactions between the lungs and the brain
The lung It is the most important surface we exchange with the environment when it comes to oxygen supply. Microbial flora that has not been researched much so far are present in this transition, which is referred to as the lung microbiome. A German research team has now, for the first time, been able to establish a close relationship between this microbiome and brain point out
Researchers from the Institute of Neuroimmunology and Multiple Sclerosis Research at the University Medical Center Göttingen (UMG) have documented for the first time how the microbial flora of the lungs controls the immune predisposition of the brain. These reactions can also be a cause of devastating autoimmune inflammation. The results of the research work were recently published in the famous journal “natureChest.
Lung flora was closely examined for the first time
All contact surfaces that people contact with the outside world are colonized with bacteria. As part of the current study, the UMG team discovered that bacterial colonization of the lungs at the contact surface between lung tissue and breathing air plays a special role.
The lung microbiome is more influential than previously thought
The team creates a new and unexpected functional connection between the lungs and the brain. Accordingly, the lung microbiome sends constant signals to the brain, causing the so-called microglia to be affected. Microglia can be considered the “immune cells of the brain”.
The study’s lead author, Dr. Leon Hosang.
The lung microbiome as an early warning system for the brain
Thus the lung microbiome acts as a species early warning system for sensitive brain tissue,” adds Professor Dr. Francesca O’Durdi, who worked alongside Professor Dr. Alexander Flugel heading the research project.
According to the research team, this little-studied relationship between the lungs and the brain could have far-reaching effects on health. For example, lung infections, antibiotic treatments, air pollution, and climate changes can alter lung flora and thus immune activity within the brain.
The lung flora is rather small compared to the intestinal flora
In recent years, many studies have examined the effect of intestinal microflora on human health. In comparison, according to the research team, the number of studies on the microbiome of the lungs is relatively small.
Possible cause of autoimmune diseases
In fact, for a long time it was believed that the lungs contained no plants at all and were sterile. The team from Göttingen showed not only that the lung flora is more influential than previously thought, but also that the smallest changes in this microbiome increase the brain’s susceptibility to disease. autoimmune diseases they change.
Antibiotics put the brain on alert
For example, researchers were able to document the way the lung microbiome sends a signal to the brain after taking antibiotics, which puts the brain’s microglia on alert. According to the working group, “Antibiotic-mediated manipulation of the lung microbiome has been associated with clearly measurable and even microscopically visible changes in microglia.”
Additionally, according to the study, microglia reacted less strongly to inflammatory signals, resulting in reduced recruitment of immune cells into inflamed brain tissue. The scientists concluded, “This explains very conclusively the low susceptibility to autoimmune inflammation.”
A new approach to treatments
According to the researchers, the microglia became paralyzed after taking antibiotics. The origin of this reaction can be traced back to a specific type of bacteria in the lungs that produce a special component of the cell wall called lipopolysaccharide.
After taking antibiotics, this cell wall component builds up in the lungs. Then the increased amount of lipopolysaccharides “paralyzed” the microglia in the brain. On the other hand, a decrease in LPS had the effect of increasing autoimmune processes in the brain.
“Maybe this is new The lung-brain axis Even their use therapeutically,” Prof. Flugel suspects. Targeted administration of probiotics or certain antibiotics could be envisaged in order to specifically influence the immune responses in the brain.
This may be the case, for example, in treating Multiple Sclerosis It plays a role, but also in general in all diseases of the central nervous system in which microglia are involved.
Similar effects through the gut-brain axis
Recently, another study demonstrated a similar association between the gut microbiome and immune responses in the brain. For more information, see the article “Gut-brain axis opens new therapeutic avenues for cancer and autoimmune diseases(FB)
Author and source information
This text complies with the specifications of the medical literature, clinical guidelines, and current studies and has been verified by medical professionals.
author:
Graduate Editor (FH) Volker Plasek
swell:
- Universitätsmedizin Göttingen: Brain-pulmonary axis: The microbial flora of the lungs controls the immune readiness of the brain (Published: February 24, 2022), European Union
- Hosang, L., Canals, R. C., van der Flier, F. J. et al. The lung microbiome regulates autoimmunity in the brain. Nature (2022). https://doi.org/10.1038/s41586-022-04427-4, Nature.com
- Hiltensperger, M., Beltrán, E., Kant, R. et al. Helper T-cell subsets imprinted on the skin and intestines show distinct functional patterns in CNS autoimmunity: In: Nature Immunology (2021), Nature.com
important note:
This article contains general advice only and should not be used for self-diagnosis or treatment. It cannot replace a visit to the doctor.

“Total coffee aficionado. Travel buff. Music ninja. Bacon nerd. Beeraholic.”








More Stories
Artemis 2’s Orion Heat Shield Faces Critical Test as Astronauts Prepare for Fiery Earth Reentry
Coral Seeding: Artificial Insemination Makes Coral More Heat Tolerant
Fear, Anger, and Denial: How People Respond to Climate Change – Research