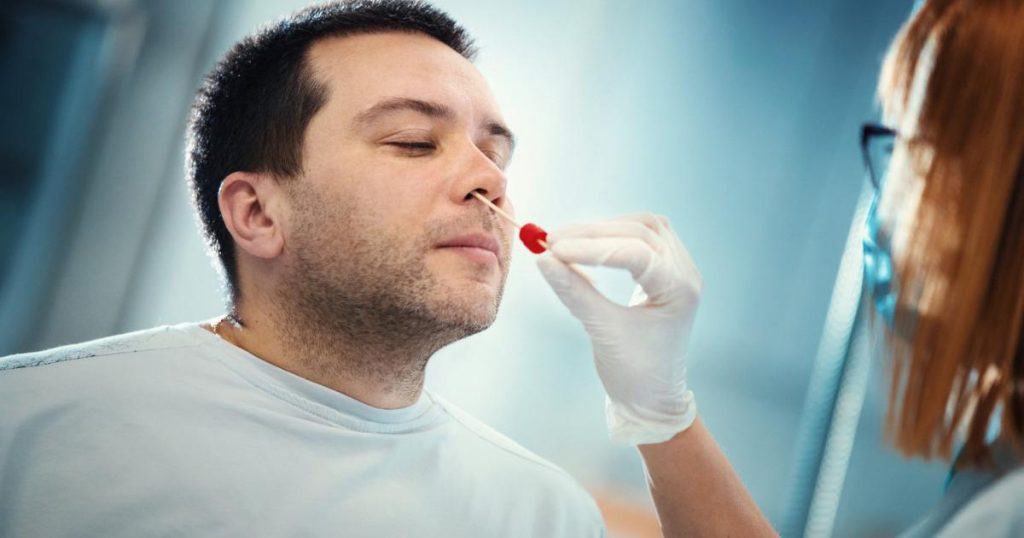
In general, the data from the current review indicate inflammation in the olfactory epithelium, in the olfactory bulb, or in both regions. X-rays show that the olfactory fissures in the upper nasal vault are not occluded in patients.
In some recovering people, this inflammation leads to a persistent deficit in olfactory ability.
Investigations are needed in the acute phase of infection
Inflammatory pathways in the nasal epithelium mainly overlap with the inflammatory signals described in some dementia patients.
Although it is not yet possible to demonstrate a definitive link between chronic or permanent smell impairment and future neurosensitivity, some studies suggest a link.
“We suspect that people who have recovered from Covid-19 who have a chronic, recurrent or permanent olfactory disorder have an increased likelihood of long-term neurological sequelae or neurodegenerative disorders.”
Inflammatory stimulation from the olfactory epithelium (the tissue of the nasal mucosa in the region of the roof of the nose) to the olfactory bulb and its associated brain regions can accelerate the development of neurodegenerative diseases.
Persistent olfactory disturbances with or without perceptual abnormalities (parosmia or placebo) after SARS-CoV-2 infection can serve as a marker to identify people with an increased long-term risk of neurodegenerative disease.
The researchers said MRI scans of people who lost smell during the acute phase of SARS-CoV-2 infection would help fill in the knowledge gaps. scalpel. Clinical studies may also be useful to determine whether certain active substances reduce persistent disturbance of the sense of smell.

“Total coffee aficionado. Travel buff. Music ninja. Bacon nerd. Beeraholic.”








More Stories
Artemis 2’s Orion Heat Shield Faces Critical Test as Astronauts Prepare for Fiery Earth Reentry
Coral Seeding: Artificial Insemination Makes Coral More Heat Tolerant
Fear, Anger, and Denial: How People Respond to Climate Change – Research